Who is behind the pelvic floor concept?
Katja von Boetticher M.Sc. Phys
As a physiotherapist, I not only advise and support you on topics such as “pelvic floor health and training” but also explain the functional connections between muscles, breathing, and movement.
I have many years of experience from my 20 years as a physiotherapist in the fields of prevention, sports, and rehabilitation. I completed my training and studies in Germany. My areas of specialization in therapeutic care include:
- Traumatology:
- Restricted shoulder movement
- Facial and jaw pain
- Hip and lower back pain
- Internal Medicine:
- COPD
- Diabetes mellitus type 2
- (Gynecological) Urology:
- Pelvic floor weakness
- Incontinence issues
We will work with you to develop your individual therapeutic program.
What is the pelvic floor concept?
Our Approach
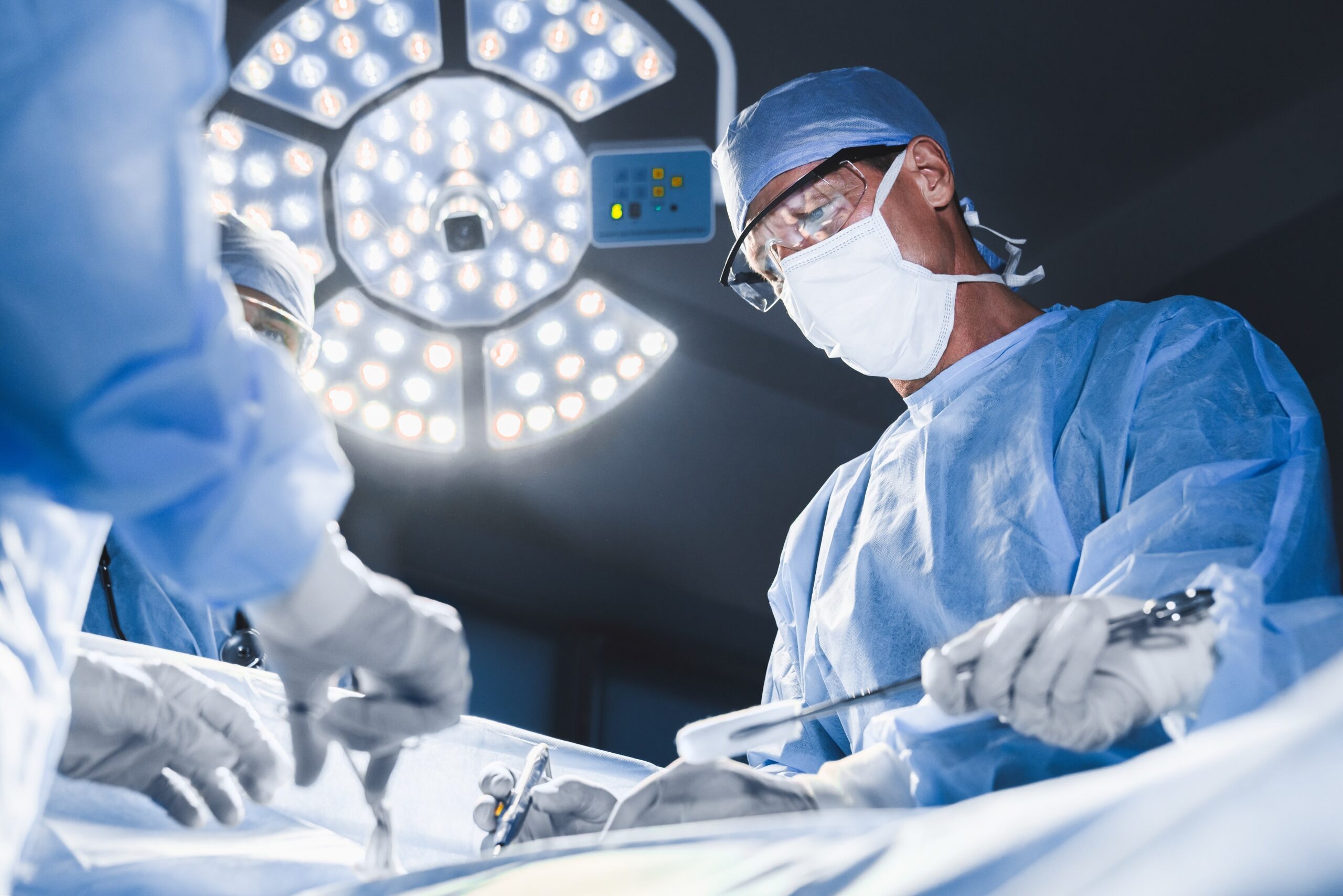
Physiotherapy is an essential component of our holistic approach to treating unresponsive pelvic floor sphincter muscles (pelvic floor sphincter dysfunction).
Moreover, this is by no means a problem exclusive to “older people.”
It is justified and understandable to ask what physiotherapy can contribute in the field of (gynecological) urology and what functional, mental, and psychological skills can be learned for self-control within the therapeutic framework.
That’s right. Self-control skills and active cooperation are necessary to achieve positive effects in this highly sensitive area. The goal is not only to reduce suffering but, above all, to enable participation in everyday and social activities.
With this motivation, we make use of various recognized therapeutic approaches, such as the Tanzberger® Concept or the Physio Pélvica® Concept.
What does “holistic” truly mean?
In holistic medicine/therapy, we look at the person as a whole. However, this is not only done through objective (visible) tests or mere observation from the “outside.” We are also daily exposed to psychological stress or hormonal changes, which, in turn, also affect our bodily structures.
In pelvic floor therapy, in particular, the causes must be recognized, and not just the symptoms treated. For this, your cooperation is fundamental.
We support you with our medical and therapeutic knowledge so that you can participate more easily in social life.
We ensure that your understanding of pelvic floor health continues to grow during therapy and that we set realistic goals together.

“New” approaches surpass old concepts
For therapy, it is clear that neither gripping with the thigh muscles nor stopping urine while going to the bathroom are useful exercises for training the pelvic floor. While stopping urination can only be practiced once as a test, the thigh muscles on the inside of the leg should not be used as a compensatory aid (alibi).
The urethral (urinari) and anal (fecal) sphincters are not “clamps” but “lacerators.” You can, for example, voluntarily squeeze your eyes shut, but demanding this from the pelvic floor system would be a feat even for an intact pelvic floor (PF).
Therefore, it’s no surprise that the motivation of those affected quickly suffers if the desired success doesn’t materialize. For this reason, our goal is not only to treat you in the conventional sense but, above all, to educate, advise, and prepare you for your daily life within medical possibilities.
Isolated tension exercises only address one characteristic, and that is muscle strength. This alone does not allow for systematic information (relative to our body system) and specific reactions to functional requirements (relative to the body’s interaction and processes).
What does this mean for training?
Every day we perform a series of movements and movement combinations that are normally never practiced in the same way. When we learn, we initially follow certain guidelines, but our individual movement experience and training level mean that we all differ in our movements and, therefore, also in our control of different body structures.
In relation to our PF, this means we must think about the control and functional tasks of the PF in terms of daily living activities. Training is personalized and also includes structural activators. Our body reacts to each new movement task by adapting. Sometimes also with compensations (“supportive movements”).
Our concept combines passive therapy with functional and everyday therapy. Our body is designed in such a way that each structure has its function. Therefore, if we move too little or use some structures in an unintended way, an imbalance is created that sometimes causes more and sometimes fewer problems.
“The brain does not know the muscle, it only knows the movement.”
(John H. Jackson, neurologist)
Therefore, we look at breathing, body position/posture, any psychological stress/stressful situations, reactions to certain stimuli on the skin/muscles and fascia, surgical history, and personal goals.
Basic Aspects of Our Therapy Concept
Our therapy focuses on a holistic approach to pelvic floor health, integrating several key components to ensure effective and lasting results.
Functional Practice and Reprogramming
A core aspect of our therapy is the specific practice of function. Movements that you want to become automatic must first be consciously practiced and integrated into your daily life. Our goal is to reprogram your system for proper function.
The Power of Breathing
Breathing exercises are another vital component. Diaphragmatic breathing movements provide rhythm, dynamic force, and direction to all the movable walls of your abdominal capsule. These physiological stretch-shortening cycles of breathing can effectively tone your muscles.

Addressing Cognitive and Emotional Factors
We also address cognitive behavior. Psychological tension, such as anxiety, can increase bladder muscle tone and the excitability of bladder wall sensors. This often creates a vicious cycle, leading to strategic avoidance behaviors like precautionary bathroom visits or limiting fluid intake. Understanding these phobic strategies is crucial for successful therapy.
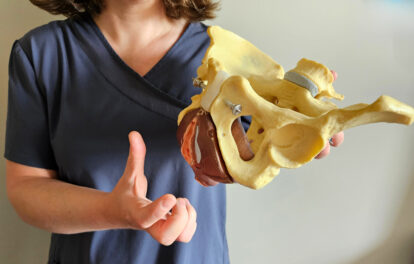
Understanding Your Body: Anatomy and Physiology
To empower you, we utilize models, images, and videos to explain the anatomy and physiology of the urogenital tract, pelvic floor (PF), and sphincter muscles. Briefly discussing these points during therapy helps you visualize and understand your body’s systems better.
Enhancing Perception and Awareness
Training your perception is key. We consider various dimensions of attention (intensity, capacity, and duration) during therapy. We’ll assess how long and to what extent you can concentrate, especially under pressure or stressful situations. Gentle questions about your sensations and feelings, such as those related to breathing movements, are used to enhance this awareness.
The Fascial System and Its Role
The fascial system is another crucial element integrated into our pelvic floor therapy. This functional network extends throughout your entire body, and its consistency is essential for smooth movement sequences. Scientific studies have proven its existence and function, highlighting four essential pathways.
The biomechanically designed pelvic floor suspension is a critical factor for continence, especially during sudden increases in pressure, like coughing, sneezing, or laughing. It’s important to understand that this spring effect must be maintained, but not by preventively tensing the pelvic floor. This pre-tension, for instance before a cough, can lead to a dysfunctional tension block.
Fascia thrives on pressure, twisting, pushing, movement, and pulling. Therefore, we often begin by preparing these structures using passive treatment methods before moving on to active therapy.
Active and Equipment-Based Therapy
Active therapy includes not only common “large” movement exercises but also the strengthening and activation of small muscles (segmental stabilization) that support and protect your joints. These muscles respond particularly well during balance, holding, and support exercises. You’ll learn direct activation techniques during your therapy sessions.
For equipment-based physiotherapy, we use tools like Thera-bands, Pezziball, Redondo ball, fascia rolls, and other small equipment. These items are easily accessible for home training, either through sports stores or directly from us.
If needed, we may also utilize Kinesio taping.

Assessment and Monitoring
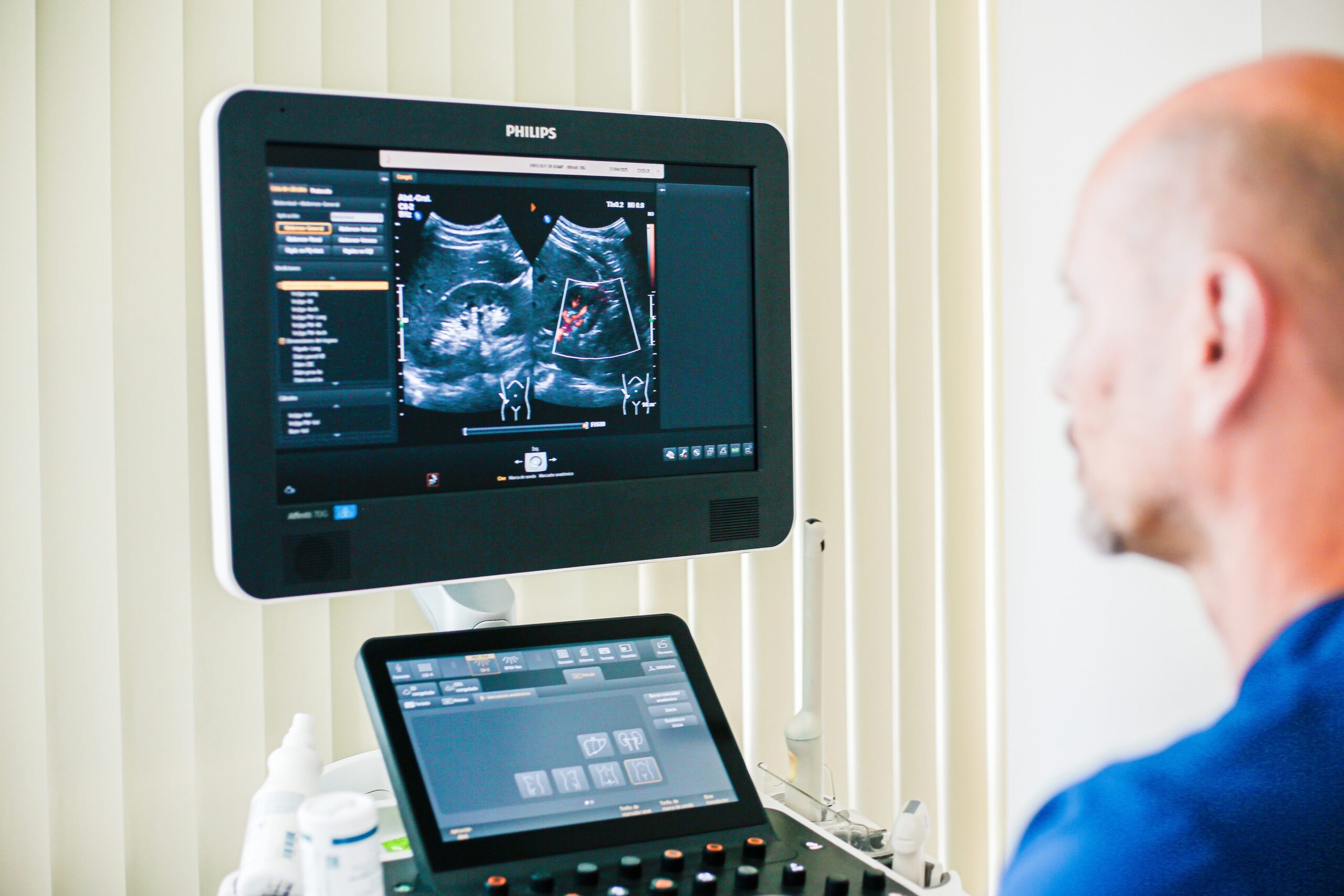
Naturally, your physiotherapeutic treatment begins with a preliminary medical examination and a therapeutic evaluation, which includes biofeedback. Biofeedback is an imaging diagnostic technique that records the activity of your pelvic floor sphincter system and helps us monitor your treatment progress.
We also evaluate and compare your postural state after each series of treatments. This allows us to see how your training has affected your posture, which, in turn, impacts your pelvic floor.
Upon request, we can also prepare a final physiotherapy report.
Ongoing Support
Our online program provides additional motivational support, making it easier for you to implement exercises consistently at home.
We are always happy to advise you and discuss possibilities in a preliminary medical consultation.